When you think about your health, what comes to mind?
Maybe your diet, exercise routine, sleep, or stress levels.
But what about your oral health?
Many people think of oral health as something separate from the rest of the body. But the reality is that the health of your mouth is closely connected to the health of your entire body.
Your mouth plays an important role in several major body systems, including:
Digestion
The immune system
Inflammation regulation
The gut microbiome
In fact, the mouth is the beginning of the digestive system and is one of the most microbially dense environments in the body. One of the main reasons the mouth has such a strong influence on overall health is because of the microorganisms that live there, which are collectively known as the oral microbiome.
The Oral Microbiome: A Complex Ecosystem
Just like the gut, the mouth has its own microbiome, which is a community of microorganisms that live in a particular environment.
According to research from the Human Microbiome Project, the human oral microbiome contains more than 700 species of bacteria, fungi, and viruses.¹
These microorganisms live on our:
Teeth
Gums
Tongue
Cheeks
Saliva
Many of these microorganisms are beneficial and help keep our mouths balanced. However, when this balance becomes disrupted, the levels of certain bacteria can increase and contribute to inflammation and disease.
Research from the Human Microbiome Project also found something interesting: oral bacteria and stool bacteria overlap by nearly 45%. This finding highlights the close connection between the mouth and the digestive system.
The Role of Saliva
Saliva also plays an important role in this relationship.
The body produces roughly 0.75 to 1.5 liters of saliva each day, and saliva continuously carries microorganisms from the mouth into the digestive tract.
In a healthy, balanced microbiome, this process is harmless. But when oral bacteria become imbalanced, this can impact:
Gut microbiome balance
Inflammation levels
Immune system regulation
Because of this connection, maintaining a healthy oral microbiome helps support overall health.
Dental Plaque and Biofilms
One of the most important factors affecting oral health is dental plaque. Plaque is often thought of as a sticky buildup on the teeth. But actually, plaque is a dense community of microorganisms.
Dental plaque contains roughly 100 billion organisms per gram, making it one of the densest microbial environments in the human body.
Dental plaque also secretes something called a biofilm.
What is a Biofilm?
A biofilm is a protective structure that allows bacteria to:
Attach to surfaces like the teeth and gums
Communicate with each other
Protect themselves from the immune system
Resist antibiotics and other antimicrobial treatments
In fact, bacteria inside biofilms can be 1,000 to 1,500 times more resistant to antibiotics compared to bacteria outside a biofilm.² And as of 2023, more than 80% of bacterial infections are caused by bacterial biofilm formation.³
But biofilms aren't only seen in the mouth. They're also involved in many infections throughout the body, including:⁴
Urinary tract infections
Bladder infections
Infective kidney stones
Chronic wounds
Diabetic foot ulcers
Otitis media (an inner ear infection)
Tonsillitis
Chronic sinusitis
Infective endocarditis (an infection of the valves of the heart)
Necrotizing fasciitis (a serious skin infection that causes tissue death)
Bacterial vaginitis (a vaginal infection)
Airway infections in those with cystic fibrosis
Catheter-associated infections
Medical device infections
In the mouth, however, biofilm formation allows harmful bacteria to accumulate along the gum line. When this happens, a condition called gingivitis can develop.
Gingivitis and Periodonitis (Periodontal Disease)
When plaque and biofilms build up along the gums, the body's immune system responds by sending white blood cells and other immune cells to the area. This creates inflammation in the gums.
If not properly managed, this inflammation can lead to gum disease, which is formally known as periodontal disease.
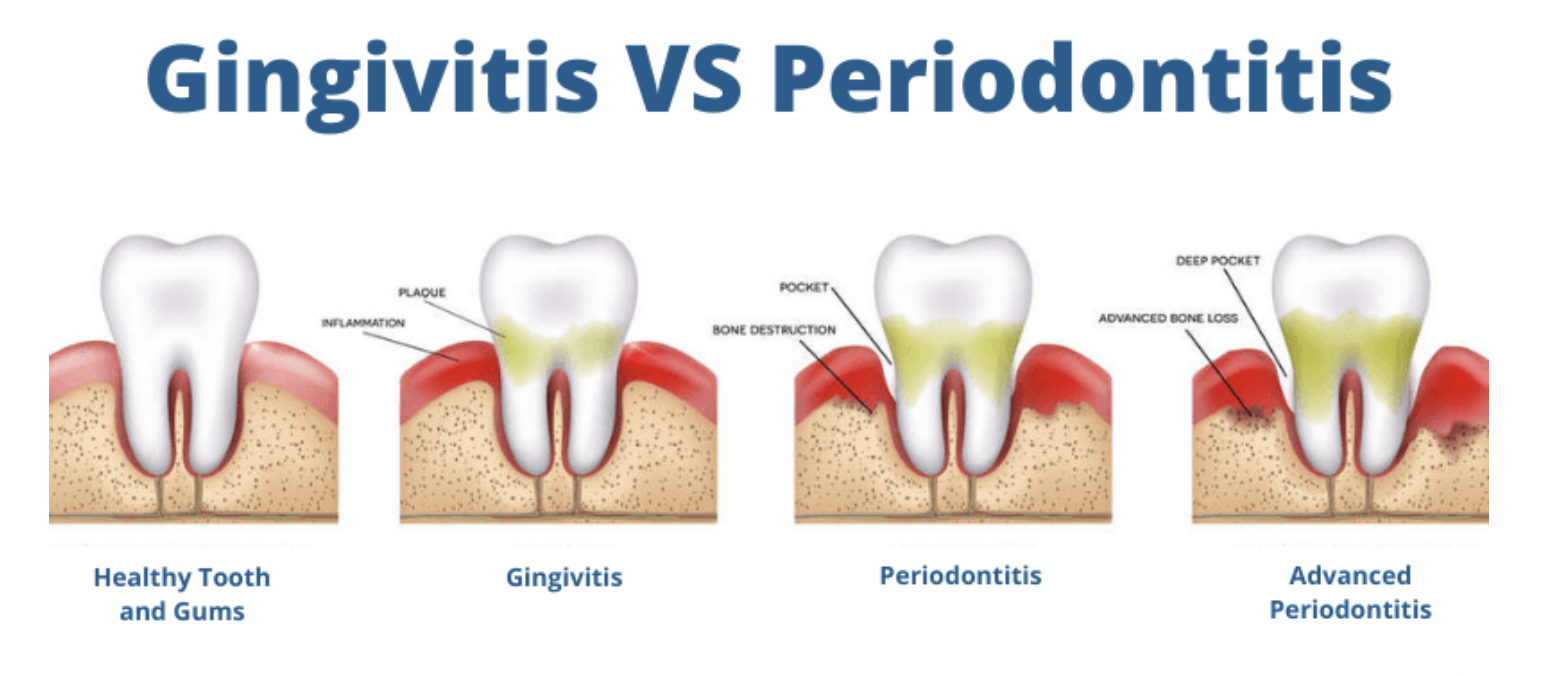
There are two main stages of periodontal disease: gingivitis and periodontitis.
Gingivitis vs Periodontitis⁵
Gingivitis
The earliest stage of periodontal disease is called gingivitis. Gingivitis occurs when the gums become inflamed due to bacterial build up along the gum line. Common symptoms of gingivitis include:
Redness
Swelling
Bleeding when brushing or flossing
Bad breath
At this stage, the condition is still reversible with proper oral hygiene and professional dental care.
Periodontitis
If gingivitis is not treated, it can progress to periodontitis, which is a more serious inflammatory condition.
Periodontitis occurs when inflammation spreads deeper into the tissues that support the teeth, including the bone and connective tissue. As the disease progresses, the healthy tissues holding teeth in place are damaged, and tooth loss can occur.
Dentists often monitor gum health by measuring periodontal pockets, which are spaces between the teeth and gums. Healthy pockets are 1-3mm in size, and pockets larger than this may indicate infection.
Because periodontal disease often develops slowly and without pain, many people don't realize they have it until it becomes advanced.
The Link Between Oral Health and Systemic Disease
Although periodontal disease begins in the mouth, its effects have been shown to extend throughout the entire body.
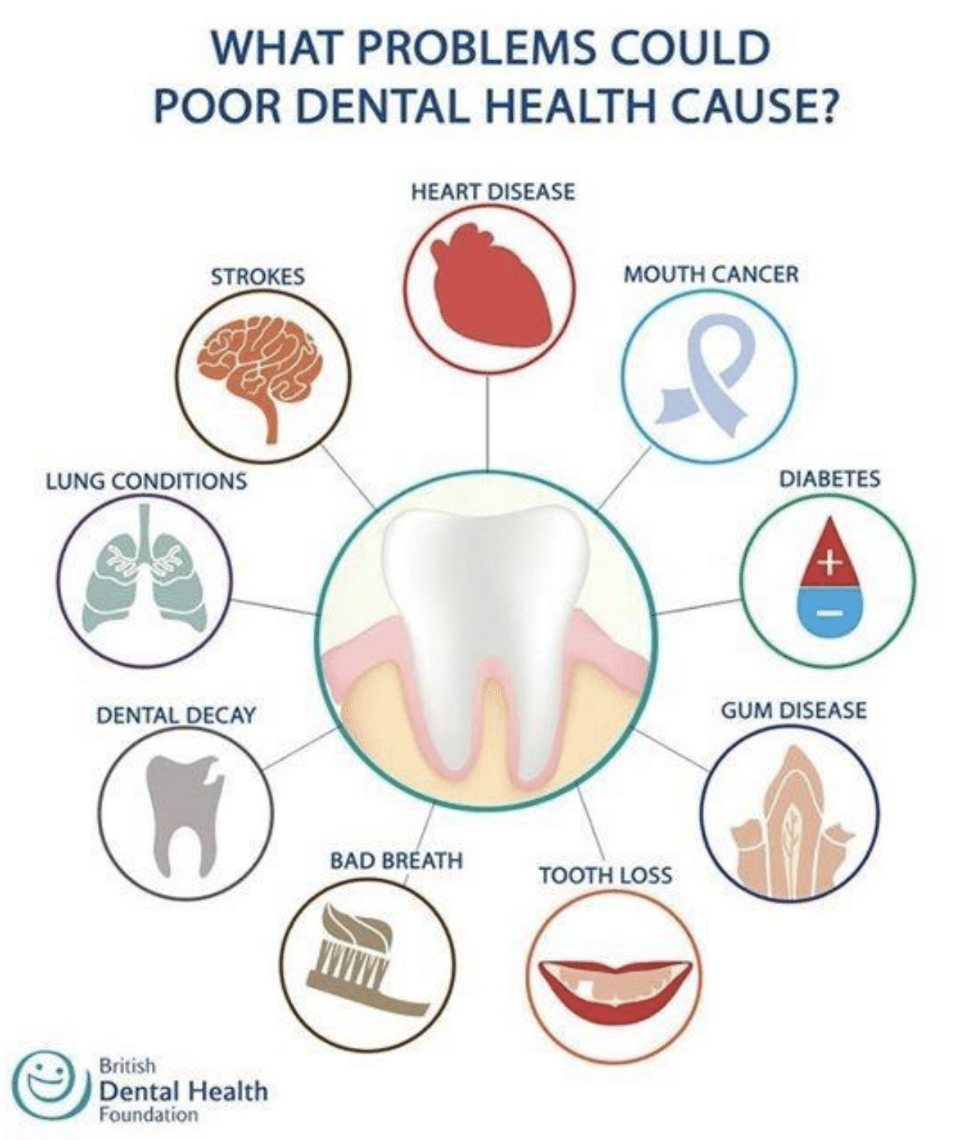
Research has shown that having periodontal disease is associated with an increased risk of several health conditions including:⁶
Diabetes
Cardiovascular disease (heart attack and stroke)
Alzheimer's disease
Pregnancy complications such as preterm birth and low-birth weight infants
Chronic periodontitis can also worsen conditions like insulin resistance, obesity, and high blood pressure due to the inflammatory stress it places on the body.
The Oral Health Foundation⁷
The Role of Oral Bacteria
One organism that's commonly linked to periodontal disease is Porphyromonas gingivalis.
This bacterium is part of the oral microbiome and can be found in many people’s mouths in small amounts. However, if the oral microbiome becomes imbalanced due to dental plaque and biofilm formation, the levels of Porphyromonas gingivalis can increase.
Certain factors can increase the chance of increased growth of Porphyromonas gingivalis, including diabetes, smoking, and conditions where the immune system is suppressed like HIV.⁸
Research has shown that this organism may contribute to disease by:⁹
Increasing inflammation throughout the body
Releasing toxins called endotoxins
Disrupting the balance of the gut microbiome
Contributing to activation of the immune system
Interestingly, Porphyromonas gingivalis has been detected in brain tissue during autopsies of people with Alzheimer's disease. This reinforces an important concept: the mouth is not separate from the rest of the body.
Instead, the mouth is part of an interconnected system involving the digestive tract, immune system, and inflammatory pathways.
Oral Health and the Immune System
The mouth is also closely connected to the immune system.
Under healthy conditions, the immune system in the mouth maintains a careful balance between helpful and harmful microorganisms. However, when conditions like plaque build up or periodontal disease cause the oral microbiome to become disrupted, the immune system can become overactivated.
This may lead to:¹⁰
Chronic inflammation in the gums
Increased inflammatory signals throughout the body
Greater stress on the immune system
Mast Cells and Oral Inflammation
The immune system contains many different types of cells that help the body respond to infections and inflammation. One of these immune cells is called a mast cell.
Mast cells are found in many tissues throughout the body, including the gums and oral tissues. These cells release inflammatory chemicals that help the body respond to injury or infection.
Research has shown that mast cells are involved in periodontal disease. When the gums become infected or inflamed, mast cells release substances that contribute to inflammation in the surrounding tissues.¹¹
In people with chronic periodontal disease, higher numbers of mast cells have been found in inflamed gum tissue. This suggests that mast cells may play a role in the inflammatory processes involved in periodontal disease.
Because chronic gum inflammation can continuously stimulate the immune system, maintaining good oral health may help reduce this potential source of inflammation in the body.
Oral Health and Viral Illness
Oral health may also influence how the body responds to viral infections.
Research from dentist Dr. Victoria Sampson found that people with poor oral health, especially periodontal disease, may have higher levels of harmful bacteria in their mouths.¹²
During illnesses like COVID-19, these bacteria may be more easily inhaled into the lungs. When this happens, they can cause secondary bacterial infections like pneumonia.
The study conducted by Dr. Sampson found that secondary bacterial infections were found in 50% of patients who died in the hospital with COVID-19. Plus, 70-74% of patients admitted into the hospital with COVID-19 required antibiotics for secondary bacterial infections.
Dr. Sampson also noted that many of the health conditions linked to more severe COVID-19 outcomes were also associated with poor oral health. These health conditions include:
Diabetes
High blood pressure
Heart disease
Obesity
This doesn't necessarily mean that periodontal disease causes severe illness. Instead, this research highlights how oral health affects overall health and our ability to fight off infections like COVID-19.
Why Oral Health Matters for Your Whole Body
The mouth plays a much larger role in health than many people realize.
The oral microbiome is closely connected to the digestive system, immune system, and inflammatory pathways throughout the body. Chronic inflammation in the mouth, like with periodontal disease, can increase the risk of inflammation and certain diseases elsewhere in the body.
Maintaining good oral health isn’t just about preventing cavities or tooth loss: it’s also an important part of supporting overall health and preventing chronic illness.
In the next blog, we'll take a closer look at the hidden sources of oral inflammation, including cavitations, and discuss how certain dental materials like metals may influence oral health.
FAQs: The Connection Between Oral Health and Overall Health
-
Yes. The mouth is closely connected to the digestive system and immune system. When harmful bacteria build up in the mouth, especially with periodontal disease (gum disease), they can trigger inflammation that may affect other parts of the body. Research has linked periodontal disease with conditions such as heart disease, diabetes, and even Alzheimer's disease.
-
The oral microbiome is the community of bacteria, fungi, and other microorganisms that live in the mouth. The mouth contains more than 700 species of microbes, many of which are beneficial and help maintain balance. However, when this balance is disrupted, harmful bacteria can increase and contribute to inflammation and periodontal disease (gum disease).
-
The earliest signs of periodontal disease (gum disease) is called gingivitis. Common symptoms include:
Red or swollen gums
Bleeding when brushing or flossing
Tender gums
Persistent bad breath
Gingivitis is often reversible if treated early with good oral hygiene and professional dental care.
-
Yes. Some dental issues, such as chronic infections or inflammation in the jaw, may not always cause obvious symptoms but can still affect the body. In the next article, we'll explore these hidden sources of inflammation, including cavitations and certain dental materials, and how they may impact oral health.
References:
1. Nitric Oxide Donor Modulates a Multispecies Oral Bacterial Community-An In Vitro Study – (nih.gov)
2. Periodontitis – (nih.gov)
3. Understanding bacterial biofilms: From definition to treatment strategies – (nih.gov)
4. Strategies for combating bacterial biofilm infections – (nih.gov)
5. Gingivitis vs Periodontitis: Stages of Gum Diseases Explained – (dayodental.com)
6. Periodontal Disease – (nih.gov)
7. Oral Health Foundation – (dentalhealth.org)
8. Porphyromonas gingivalis Virulence Factors and Clinical Significance in Periodontal Disease and Coronary Artery Diseases – (nih.gov)
9. Porphyromonas gingivalis, a Long-Range Pathogen: Systemic Impact and Therapeutic Implications – (nih.gov)
10. Periodontitis and Systemic Inflammatory Multimorbidity: Narrative Review of Literature – (nih.gov)
11. Mast cells and oral inflammation – (nih.gov)
12. Could there be a link between oral hygiene and the severity of SARS-CoV-2 infections? – (nih.gov)